Treating, curing and preventing disease — WJEC GCSE Study Guide
Exam Board: WJEC | Level: GCSE
This topic explores the vital mechanisms we use to fight communicable diseases, from the preventative power of vaccines to the curative role of antibiotics. Understanding how these work, alongside the rigorous process of drug development, is crucial for exam success as it frequently appears in high-mark extended response questions.
## Overview
Topic 3.3, *Treating, Curing and Preventing Disease*, is a cornerstone of the GCSE Biology specification. It bridges the gap between microscopic cellular processes and global public health. You will learn how we harness the body's own immune system through vaccination, how we use antibiotics to destroy bacterial invaders, and why the rise of antibiotic resistance is one of the greatest threats to modern medicine.
This topic connects heavily with your prior knowledge of cell structure (specifically the differences between bacterial, viral, and human cells) and natural selection. Examiners love to test this area using application questions, often presenting you with data from clinical trials or asking you to explain the mechanism of a new vaccine. Mastering the precise terminology here—such as distinguishing between antigens and antibodies—is essential for securing top marks.
## Key Concepts
### Concept 1: Vaccination and Immunity
Vaccination is a preventative measure designed to protect individuals from communicable diseases before they become infected. The process relies on the remarkable memory of the human immune system.
A vaccine contains a dead, weakened, or inactive form of a pathogen. Crucially, it contains the **antigens**—the unique protein markers found on the surface of that specific pathogen. When injected, these antigens are detected by your white blood cells (specifically B-lymphocytes).
Recognising the antigens as foreign, the white blood cells are stimulated to produce **antibodies**. These are Y-shaped proteins that are perfectly complementary to the specific antigen, fitting together like a lock and key. The antibodies bind to the antigens, clumping the pathogens together and marking them for destruction by other white blood cells (phagocytes).
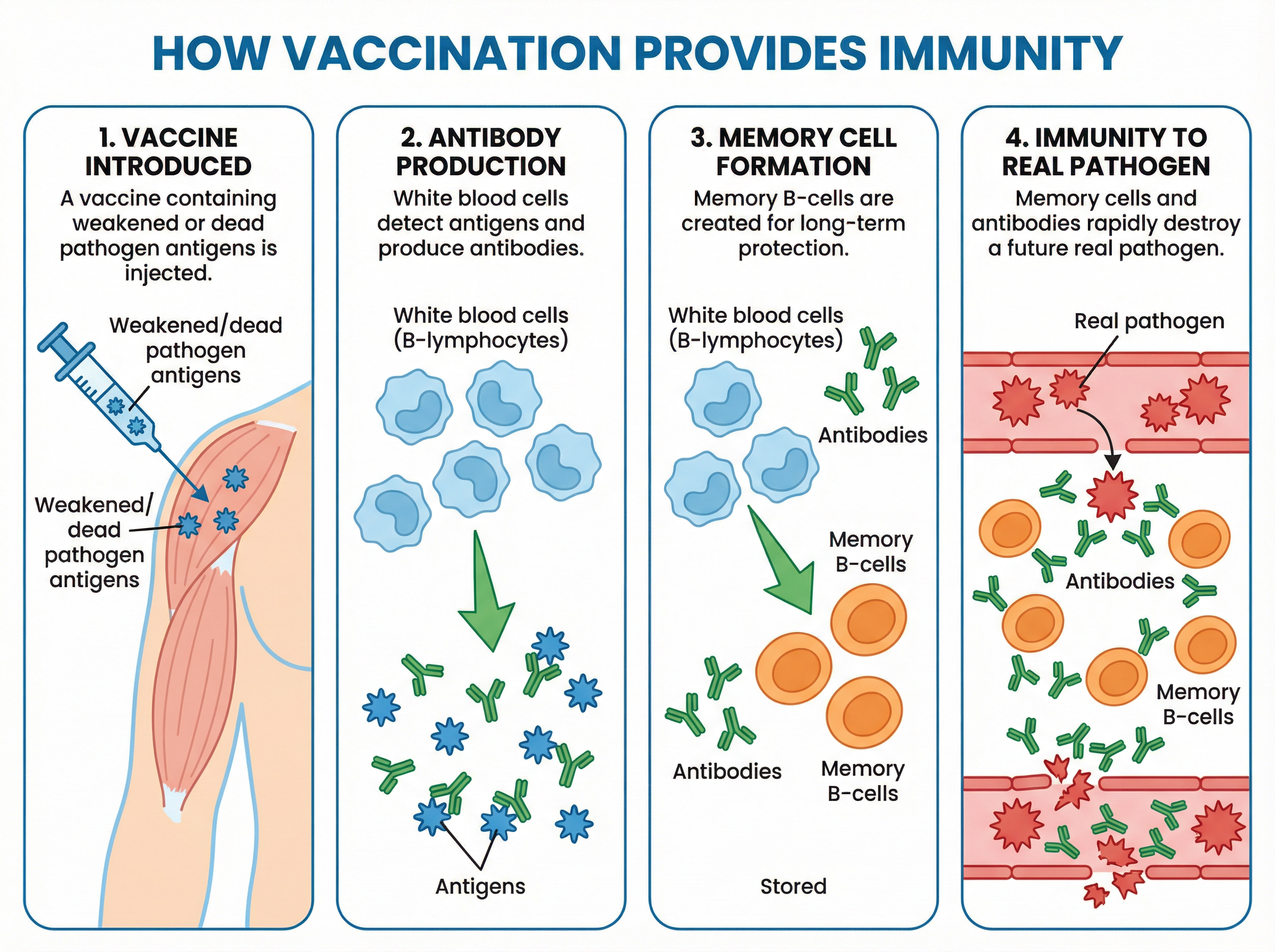
The true power of vaccination lies in what happens next. After the initial response, some of the white blood cells remain in the blood as **memory cells**. If the real, live pathogen enters the body months or years later, these memory cells recognise the antigen immediately. They rapidly produce a massive quantity of the specific antibodies, destroying the pathogen before it can reproduce and cause symptoms. This state of readiness is called **immunity**.
**Herd Immunity**: If a large enough percentage of a population is vaccinated, the spread of the pathogen is significantly reduced. This protects vulnerable individuals who cannot be vaccinated, such as newborn babies or those with compromised immune systems.
### Concept 2: Antibiotics and Painkillers
When prevention fails and a bacterial infection occurs, we turn to curative medicines: antibiotics.
**Antibiotics** (such as penicillin) are medicines that kill infective bacteria inside the body or prevent them from reproducing. They work by targeting specific structures or processes unique to bacterial cells, such as disrupting the formation of the bacterial cell wall. Because human cells do not have cell walls, the antibiotic destroys the bacteria without harming the patient's own tissues.
**Crucial Exam Point**: Antibiotics **cannot** kill viruses. Viruses reproduce *inside* the host's cells. It is extremely difficult to develop drugs that kill viruses without also damaging the body's tissues.
**Painkillers** (such as paracetamol or aspirin) and other symptom-relieving drugs are entirely different. They treat the *symptoms* of the disease (like a headache or fever) to make the patient feel better, but they do not kill the pathogens causing the disease.
### Concept 3: Antibiotic Resistance
One of the most frequent exam topics is the development of antibiotic-resistant bacteria, such as MRSA. This is a classic example of natural selection occurring in real-time.
Within a population of bacteria, there is natural variation due to random genetic mutations. Occasionally, a mutation may give a bacterium resistance to a specific antibiotic. When the patient takes that antibiotic, the non-resistant bacteria are killed. However, the resistant bacterium survives.
Because the competition for resources (like nutrients and space) has been removed, the resistant bacterium rapidly reproduces. It passes on the allele for resistance to its offspring. Over time, the entire population becomes resistant, and the antibiotic is no longer effective.
To slow down the rate of resistance development, doctors must avoid over-prescribing antibiotics (e.g., not giving them for viral infections), and patients must complete the full course of antibiotics to ensure all bacteria are killed.
### Concept 4: Drug Discovery and Development
Historically, many drugs were extracted from plants and microorganisms. For example, the heart drug digitalis originates from foxgloves, the painkiller aspirin originates from willow, and penicillin was discovered by Alexander Fleming from the *Penicillium* mould.
Today, most new drugs are synthesised by chemists in the pharmaceutical industry. However, before a new drug can be prescribed, it must undergo a rigorous testing process to ensure it is safe and effective.
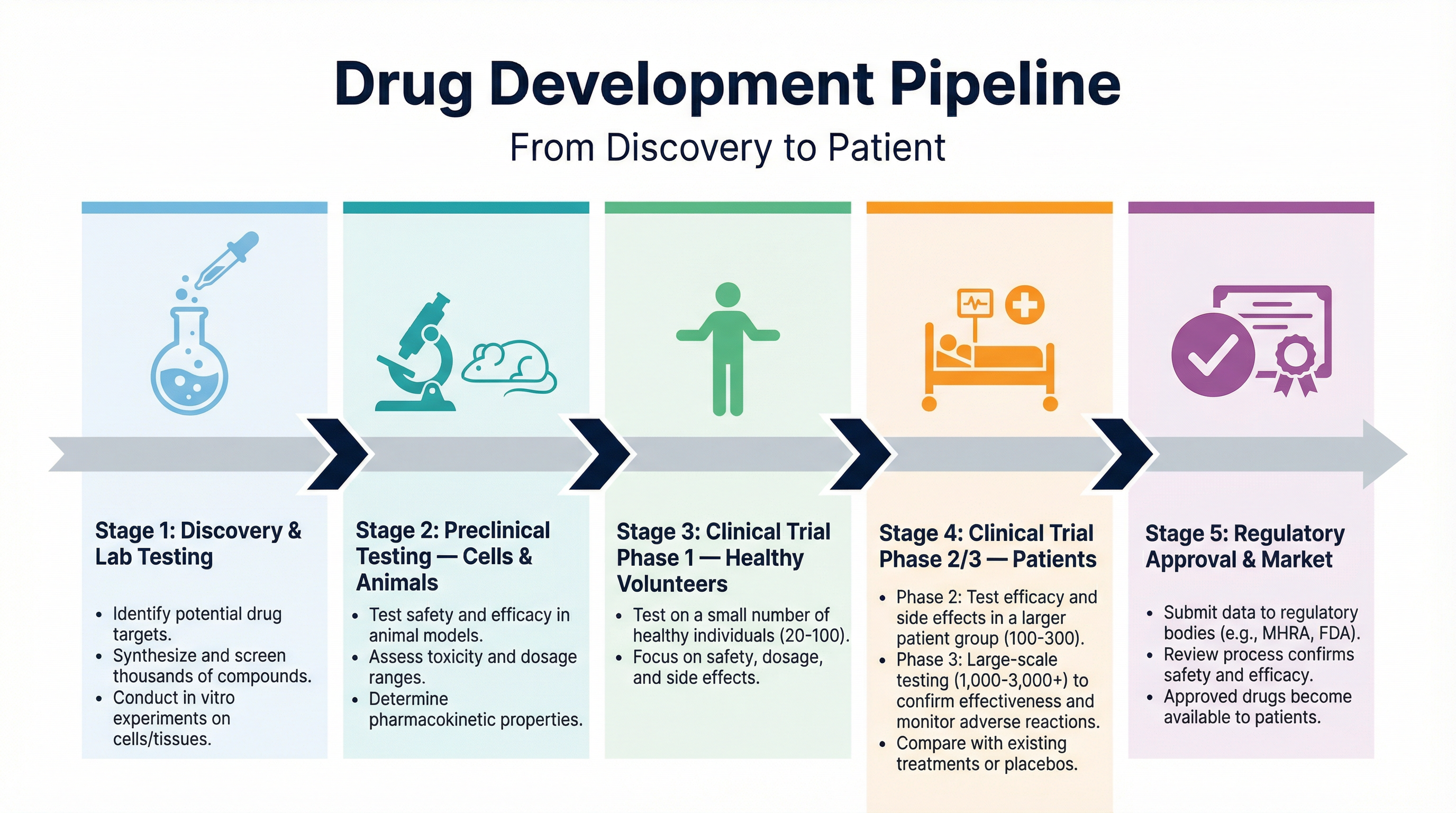
The process follows a strict sequence:
1. **Preclinical Testing**: The drug is tested in laboratories using cells, tissues, and live animals. This stage evaluates the drug's toxicity (is it safe?) and efficacy (does it work?), and helps determine a starting dose.
2. **Clinical Trials (Phase 1)**: The drug is tested on a small group of healthy human volunteers using very low doses. The primary goal here is to check for safety and side effects in a healthy body.
3. **Clinical Trials (Phase 2 & 3)**: If safe, the drug is tested on patients who have the disease. This determines the optimum dose (the dose that is most effective with the fewest side effects) and confirms efficacy.
To ensure results are reliable and unbiased, clinical trials are often **double-blind**. In a double-blind trial, patients are randomly divided into two groups. One group receives the active drug, and the other receives a **placebo** (a dummy drug that looks identical but contains no active ingredient). Crucially, neither the patients nor the doctors know who is receiving which treatment until the trial is complete. This eliminates psychological bias from the patients and observation bias from the doctors.
### Concept 5: Culturing Microorganisms (Aseptic Technique)
*(Required Practical Content)*
To study microorganisms, such as investigating the effect of antibiotics on bacterial growth, scientists must culture them in the lab. This involves providing the bacteria with a culture medium (like nutrient broth or agar jelly) containing carbohydrates, minerals, proteins, and vitamins.
**Aseptic technique** is a set of procedures used to prevent contamination. Contamination by unwanted microorganisms from the air or skin would ruin the experiment and could potentially culture dangerous pathogens.
Key aseptic steps include:
- Sterilising all Petri dishes and culture media before use (usually in an autoclave).
- Sterilising inoculating loops by passing them through a roaring Bunsen burner flame until red hot.
- Working close to a Bunsen burner, as the updraft prevents airborne microbes from settling on the agar.
- Securing the lid of the Petri dish with adhesive tape (but not sealing it completely, to allow oxygen in and prevent the growth of harmful anaerobic bacteria).
- Incubating the plates upside down to prevent condensation from dripping onto the agar.
In school laboratories, cultures should be incubated at a maximum temperature of 25°C. This greatly reduces the likelihood of growing pathogens that are harmful to humans, which typically thrive at body temperature (37°C).

## Mathematical/Scientific Relationships
When investigating the effect of antibiotics on bacterial growth using agar plates, you will often need to calculate the **cross-sectional area of the clear zone** (the zone of inhibition) around an antibiotic disc.
The larger the clear zone, the more effective the antibiotic.
**Formula:** Area = πr²
*(You must memorise this formula; it is not given on the biology formula sheet)*
Where:
- **π** (pi) = 3.14 (or use the π button on your calculator)
- **r** = the radius of the clear zone (measure the diameter using a ruler and divide by 2)
**Units:** Ensure your measurements are in mm. The area will therefore be in mm².
## Practical Applications
Understanding drug development is crucial for interpreting news about new medical treatments, such as the rapid development of mRNA vaccines during the COVID-19 pandemic. The principles of aseptic technique are not just for the lab; they form the basis of surgical hygiene in operating theatres worldwide, preventing life-threatening post-operative infections.