Overview
Schizophrenia is a severe mental disorder affecting approximately 1% of the population, characterised by a profound disruption of cognition and emotion. For the AQA A-Level exam, it is a major topic in the "Issues and Debates in Psychology" section of Paper 3. Examiners expect candidates to demonstrate a detailed understanding of classification systems, biological and psychological explanations, and various therapeutic approaches. Crucially, marks are awarded for sustained and effective evaluation, weighing up the strengths and limitations of each theory and therapy using empirical evidence. This guide will equip you with the precise knowledge and analytical skills required to excel.

1. Classification and Diagnosis of Schizophrenia
Accurate diagnosis is the foundation of effective treatment, but it is fraught with challenges regarding reliability and validity.
Key Classification Systems: Candidates must be able to distinguish between the two major systems:
- DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, 5th Edition): Published by the American Psychiatric Association. Requires at least two of five key symptoms, with one being delusions, hallucinations, or disorganised speech. The symptoms must be present for at least six months.
- ICD-10 (International Classification of Diseases, 10th Edition): Published by the World Health Organisation. Places more emphasis on Schneider's first-rank symptoms. Two or more negative symptoms are sufficient for diagnosis. Tends to result in a higher rate of diagnosis than DSM-5.
Evaluation of Diagnosis:
- Reliability: Refers to the consistency of diagnosis. Cheniaux et al. (2009) found very low inter-rater reliability between two psychiatrists using both DSM and ICD systems, suggesting a significant weakness.
- Validity: Refers to the accuracy of diagnosis. A key issue is criterion validity; there is a high degree of symptom overlap with other disorders like bipolar disorder, which can lead to misdiagnosis.
- Co-morbidity: The presence of two or more disorders simultaneously. Buckley et al. (2009) found that around 50% of patients with schizophrenia also have a diagnosis of depression, which complicates diagnosis and treatment.
- Cultural Bias: African-American and Afro-Caribbean individuals are several times more likely to be diagnosed with schizophrenia in the UK and US. This is not due to higher prevalence but likely due to cultural differences in expression of symptoms or clinician bias.
2. Symptoms of Schizophrenia
Examiners award credit for a clear distinction between positive and negative symptoms. A simple way to remember this is that positive symptoms are 'added' to a person's experience, while negative symptoms represent something 'removed' or lost.
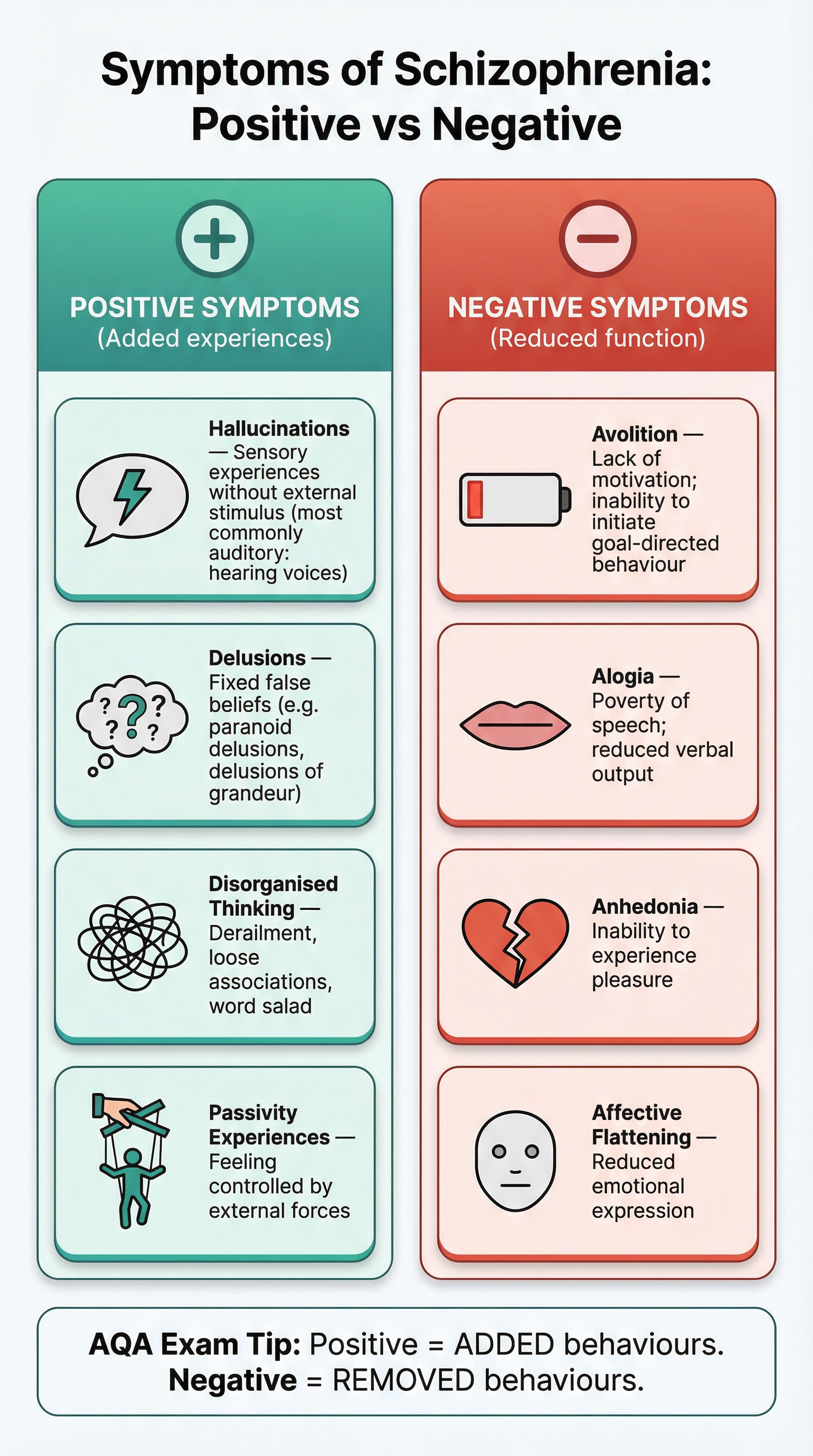
Positive Symptoms (Type I)
These are pathological excesses or distortions of normal functions.
- Hallucinations: Sensory experiences that have no basis in reality. They can be auditory (hearing voices), visual, tactile (feeling things), or olfactory (smelling things).
- Delusions: Irrational beliefs that are fixed and resistant to change, even with contradictory evidence. Common types include delusions of persecution (believing one is being conspired against) and delusions of grandeur (believing one has special powers or importance).
Negative Symptoms (Type II)
These are pathological deficits or the loss of normal functions.
- Avolition: Apathy and a lack of motivation to initiate and persist in goal-directed activities. This is often misinterpreted as laziness.
- Alogia (Speech Poverty): A reduction in the amount and quality of speech. This can manifest as brief, empty replies to questions.
- Affective Flattening: A reduction in the range and intensity of emotional expression, including facial expression, voice tone, and eye contact.
3. Biological Explanations of Schizophrenia
The Dopamine Hypothesis
This is the most prominent neurochemical explanation. You must know the difference between the original and revised versions.
- Original Hypothesis: Schizophrenia is caused by an excess of dopamine (hyperdopaminergia). Evidence came from the fact that antipsychotic drugs that block dopamine reduce symptoms, and drugs like amphetamines that increase dopamine can induce psychosis.
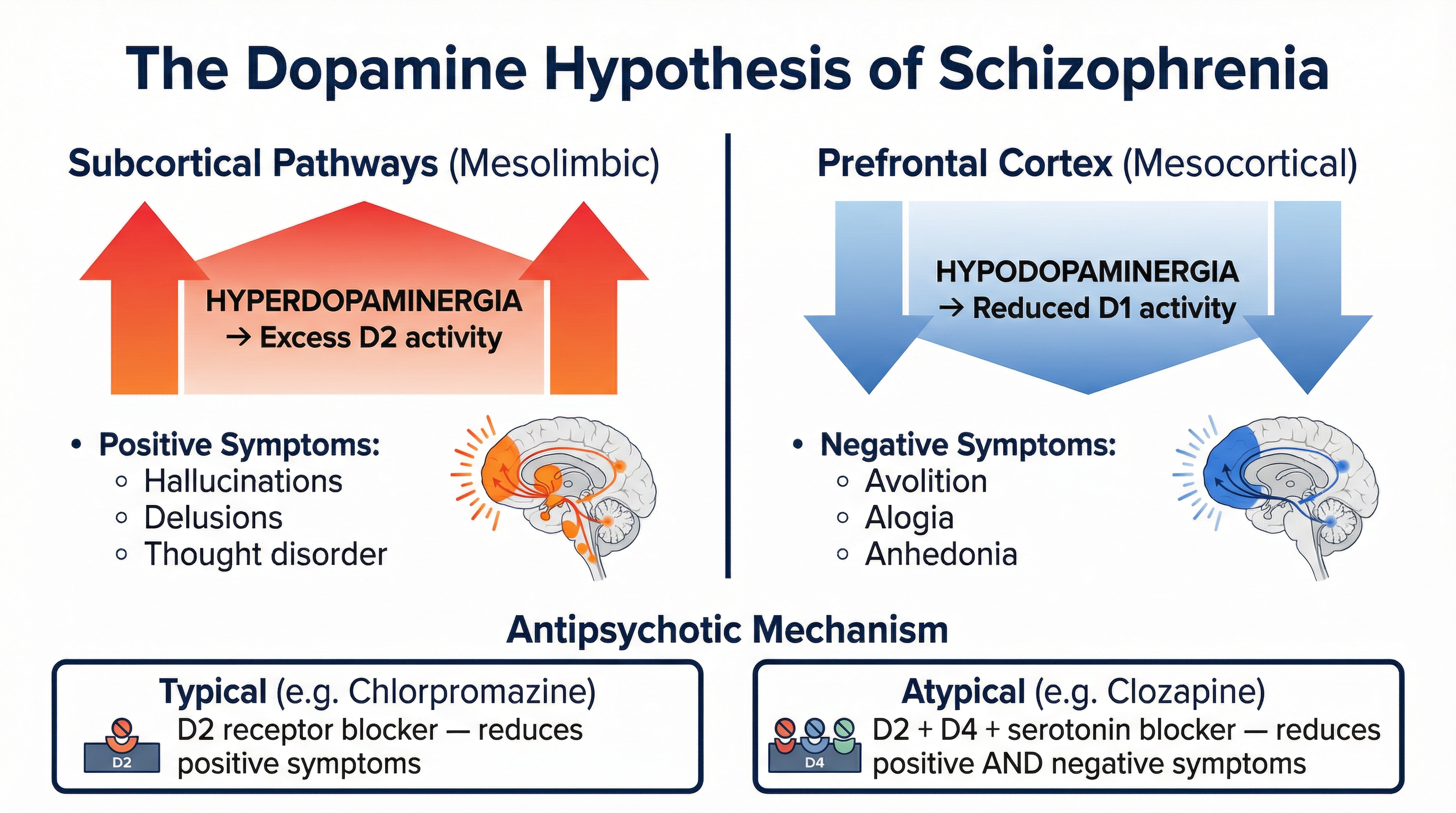
- Revised Hypothesis (Davis et al., 1991): This more nuanced version proposes that dopamine dysregulation is pathway-dependent.
- Hyperdopaminergia in the Subcortex: Excess dopamine in the mesolimbic pathway is linked to positive symptoms.
- Hypodopaminergia in the Cortex: A deficit of dopamine in the mesocortical pathway (especially the prefrontal cortex) is linked to negative symptoms.
Genetic Factors
There is a strong body of evidence suggesting a genetic vulnerability to schizophrenia.
- Family Studies: Gottesman (1991) conducted a large-scale review and found a clear relationship between genetic similarity and the shared risk of schizophrenia. MZ (identical) twins have a 48% concordance rate, while DZ (fraternal) twins have a 17% rate. This strongly suggests a genetic component, but as the MZ rate is not 100%, it cannot be the only factor.
- Candidate Genes: Schizophrenia is polygenic (requires a number of factors to work in combination). Many genes have been identified, each conferring a small increased risk. Many of these genes are associated with the production of dopamine.
Neural Correlates
These are measurements of the structure or function of the brain that correlate with an experience, in this case, schizophrenia.
- Enlarged Ventricles: Many people with schizophrenia have enlarged ventricles (fluid-filled gaps in the brain), suggesting damage or loss of brain tissue, particularly in the temporal and frontal lobes.
- Negative Symptoms and the Ventral Striatum: Juckel et al. (2006) found a negative correlation between activity levels in the ventral striatum and the severity of negative symptoms. The ventral striatum is involved in reward anticipation, and low activity here may explain avolition.
4. Psychological Explanations of Schizophrenia
Family Dysfunction
These theories place the cause of schizophrenia on abnormal patterns of communication within the family.
- Schizophrenogenic Mother: Fromm-Reichmann (1948) proposed a psychodynamic explanation where a cold, rejecting, and controlling mother creates a family climate of tension and secrecy, leading to schizophrenia. (Crucial Evaluation: This theory is outdated, has little empirical support, and is socially sensitive as it blames parents).
- Double Bind Theory: Bateson et al. (1972) suggested that children who frequently receive contradictory messages from their parents are more likely to develop schizophrenia. For example, a mother who says 'I love you' while turning her head away in disgust. This creates a confusing and internally incoherent construction of reality. (Crucial Evaluation: Also lacks strong empirical support and can be seen as parent-blaming).
- Expressed Emotion (EE): This refers to the level of criticism, hostility, and emotional over-involvement directed at the patient by their family. High levels of EE have been shown to be a significant factor in patient relapse. It is more of a maintenance model than a causal one.
Cognitive Explanations
This approach focuses on the role of mental processes.
- Frith et al. (1992) identified two kinds of dysfunctional thought processes:
- Metarepresentation Dysfunction: An inability to recognise our own thoughts and actions as being carried out by ourselves. This could explain auditory hallucinations (attributing one's own inner speech to an external source) and delusions of control.
- Central Control Dysfunction: An inability to suppress automatic thoughts and speech triggered by other thoughts. This could explain disorganised speech and thought disorder as patients cannot suppress automatic associations.
5. Therapies for Schizophrenia
Biological Therapies: Antipsychotics
- Typical Antipsychotics (e.g., Chlorpromazine): Developed in the 1950s. They are dopamine antagonists, primarily blocking D2 receptors in the mesolimbic pathway. They are effective at reducing positive symptoms but can have severe side effects (e.g., tardive dyskinesia - involuntary facial movements).
- Atypical Antipsychotics (e.g., Clozapine, Risperidone): Developed in the 1970s. They block D2 receptors but also act on serotonin and glutamate receptors. They are effective for both positive and negative symptoms and have a lower risk of extrapyramidal side effects. However, Clozapine can cause a fatal blood condition called agranulocytosis, requiring regular blood tests.
Psychological Therapies
- Cognitive Behavioural Therapy for Psychosis (CBTp): Helps patients identify and challenge their irrational thoughts. It does not eliminate symptoms but helps patients cope with them and reduce distress. For example, helping a patient to understand that their auditory hallucinations are not real and are a product of their illness.
- Family Therapy: Aims to improve communication and interaction within the family, primarily by reducing levels of Expressed Emotion (EE). It has been shown to significantly reduce relapse rates.
- Token Economies: A form of behavioural therapy used in institutional settings. Tokens are given as rewards for desirable behaviours (e.g., getting dressed). These tokens can then be exchanged for privileges. (Crucial Evaluation: Raises ethical issues as it can be seen as controlling and dehumanising. Also, benefits may not generalise to the outside world).
6. The Interactionist Approach
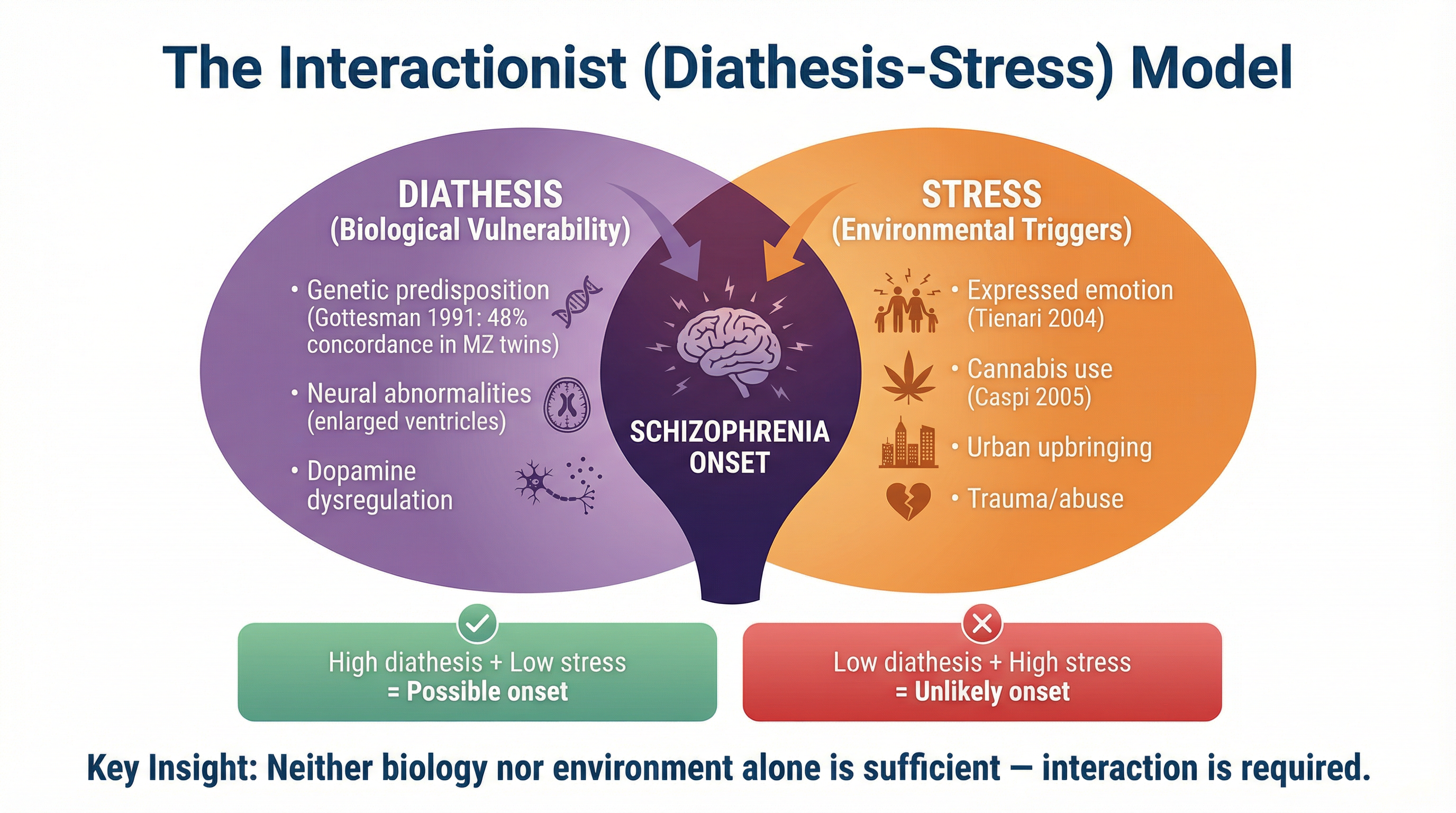
This is the most sophisticated and widely accepted approach. It acknowledges that schizophrenia is the result of an interaction between biological (diathesis) and environmental/psychological (stress) factors.
- The Diathesis-Stress Model: 'Diathesis' means vulnerability (often genetic or neurochemical), and 'stress' refers to a negative psychological experience (e.g., family dysfunction, trauma, substance abuse). The model proposes that individuals have varying levels of genetic vulnerability, which is then triggered by environmental stressors.
- Key Evidence: Tienari et al. (2004) studied adopted children of schizophrenic mothers. Those raised in families with high levels of criticism and conflict were much more likely to develop schizophrenia than those raised in healthy, supportive families. This provides direct support for the interactionist approach.
- Implications for Treatment: The interactionist model justifies the use of combination therapies, such as using antipsychotic medication to treat the biological aspects and CBTp to address the psychological aspects. This is now the standard practice in the UK.